MAC lung disease is a chronic and potentially serious lung infection caused by the Mycobacterium avium complex (MAC)—a group of genetically related bacteria commonly found in soil, water, and even household plumbing systems. Although most people are exposed to these organisms in everyday life without any consequence, some individuals—especially older adults, those with pre-existing lung conditions like bronchiectasis or COPD, or those with weakened immune systems—are more susceptible to infection.1Kumar K, Loebinger MR. Nontuberculous Mycobacterial Pulmonary Disease: Clinical Epidemiologic Features, Risk Factors, and Diagnosis: The Nontuberculous Mycobacterial Series. Chest. 2022 Mar;161(3):637-646. doi: 10.1016/j.chest.2021.10.003. Epub 2021 Oct 8. PMID: 34627854.
Among nontuberculous mycobacterial (NTM) infections, MAC is the most frequent cause of pulmonary disease worldwide, particularly due to the species M. avium and M. intracellulare.2American Lung Association. (n.d.). MAC lung disease. https://www.lung.org/lung-health-diseases/lung-disease-lookup/mac-lung-disease#:~:text=MAC%20lung%20disease%20is%20an,be%20referred%20to%20as%20MAI. Other species in this group include M. chimaera, M. colombiense, and M. marseillense, among others. These bacteria are typically not transmitted from person to person, which means the disease is not contagious. MAC lung disease can develop gradually over time and present with a persistent cough, fatigue, weight loss, shortness of breath, or recurrent respiratory infections. It may mimic tuberculosis in some cases, especially when cavities form in the lungs, but tends to progress more slowly. Early diagnosis is important, as advanced disease can cause significant lung damage and becomes harder to manage.
Causes of MAC Lung Disease
As mentioned earlier, it is caused by a group of bacteria called mycobacterium avium complex (MAC) that inhabit dust, soil, and water naturally. They’re a type of nontuberculous mycobacteria (NTM) leading to a nontuberculous mycobacteria (NTM) type of infection. MAC is a nonmotile, non-spore-forming, gram-positive acid-fast bacillus. Unlike Mycobacterium tuberculosis, which spreads from person to person, MAC organisms are thought to be acquired from the environment, most likely through inhalation of aerosolized water or soil particles. There are over 200 known species of NTM, but MAC—primarily Mycobacterium avium and Mycobacterium intracellulare—is responsible for up to 80% of NTM-related lung infections.3Griffith, D. E., Aksamit, T., Brown-Elliott, B. A., Catanzaro, A., Daley, C., Gordin, F., Holland, S. M., Horsburgh, R., Huitt, G., Iademarco, M. F., Iseman, M., Olivier, K., Ruoss, S., von Reyn, C. F., Wallace, R. J., & Winthrop, K. (2007). An official ATS/IDSA statement: Diagnosis, treatment, and prevention of nontuberculous mycobacterial diseases. American Journal of Respiratory and Critical Care Medicine, 175(4), 367–416. https://doi.org/10.1164/rccm.200604-571ST
Signs & Symptoms
MAC lung disease presents with signs and symptoms that vary and often are nonspecific. That is why diagnosis is often delayed. Some people have mild or unnoticeable symptoms. Often symptoms are not even respiratory in nature. You may experience the following symptoms:
- Chronic cough with or without mucus.
- Hemoptysis which means coughing up blood.
- Fatigue.
- Low-grade fever between 99.6 F (37.5 C) and 100.3 F (37.9 C).
- Night sweats
- Shortness of breath
- Unexplained weight loss and reduced appetite
- Chest pain
- Anxiety
Types of MAC Lung Disease
There are two types of MAC lung disease:
Nodular/Bronchiectatic MAC Lung Disease:
This form occurs predominantly in older adults, especially nonsmoking women over the age of 50. In this type, the infection spreads in the small airways and air sacs, leading to the development of small nodules that grow slowly. These are often picked up on imaging like a CT scan. The ongoing presence of the bacteria causes chronic inflammation, which damages the airway walls and leads to bronchiectasis—an irreversible dilation of the airways. This damage makes it easier for more infections to occur and harder for existing ones to clear. Chest radiographs reveal bronchiectasis, particularly in the mid-lung fields. It is slowly progressive, with patients often experiencing recurrent respiratory infections over many years before diagnosis. It is sometimes referred to as Lady Windermere syndrome when it involves specific lung zones, particularly in the right middle lobe or lingula. If left untreated, it can lead to complications such as recurrent bronchitis or pneumonia. This may also occur in patients with previously undiagnosed bronchiectasis.
Fibrocavitary Disease:
This type is seen in patients with known underlying lung disease, particularly those with a history of smoking or chronic obstructive pulmonary disease (COPD). It can also develop in areas of previous bronchiectasis, such as in patients who have had prior tuberculosis. It presents with more severe symptoms, including cough, weight loss, upper lobe infiltrates, and cavities on chest imaging, closely resembling tuberculosis. However, symptoms tend to be less severe compared to those seen in active tuberculosis, and lung destruction may be extensive by the time of diagnosis, with large cavities visible on chest radiographs.
Additionally, there are two other less common clinical forms of MAC lung disease:
Solitary Pulmonary Nodules
A less common form of MAC lung disease can present as solitary pulmonary nodules, which can resemble lung cancer. Studies have reported a relatively high frequency of this presentation in certain patient populations.4Lim J, Lyu J, Choi CM, Oh YM, Lee SD, Kim WS, Kim DS, Lee H, Shim TS. Non-tuberculous mycobacterial diseases presenting as solitary pulmonary nodules. Int J Tuberc Lung Dis. 2010 Dec;14(12):1635-40. PMID: 21144251.
Hypersensitivity Pneumonitis
Exposure to MAC, especially in environments like hot tubs, can sometimes lead to hypersensitivity pneumonitis, a type of allergic reaction. This condition, also known as “hot tub lung,” is primarily seen in immunocompetent individuals without prior lung disease. Symptoms typically improve upon avoiding the exposure, and antibiotic treatment is usually not required.5Cappelluti E, Fraire AE, Schaefer OP. A case of “hot tub lung” due to Mycobacterium avium complex in an immunocompetent host. Arch Intern Med. 2003 Apr 14;163(7):845-8. doi: 10.1001/archinte.163.7.845. PMID: 12695276.
Risk of MAC Lung Disease
MAC lung disease does not have a particular age or gender that it affects. But some people are more at risk than others. Generally, people who are at greater risk are as follows.
- People over the age of 65, particularly women in their postmenopausal years, are at a higher risk. The lack of estrogen in postmenopausal women may reduce the protective effects against infections like MAC, which could increase susceptibility.6Lee, S. Y., Kim, J. H., Kim, Y. J., & Kim, S. Y. (2019). Estrogen and Mycobacterium avium complex lung disease: Insights from clinical and animal studies. Journal of Thoracic Disease, 11(1), 1-7. https://doi.org/10.21037/jtd.2019.12.58
- A weakened immune system is another risk factor. So, people who have AIDS are at high risk if exposed to MAC.
- People who develop certain lung conditions like bronchiectasis (and conditions that can lead to bronchiectasis), chronic obstructive lung disease, etc.
Diagnosis of MAC Lung Disease
Your doctor will do your physical examination and get you checked first by asking about the symptoms you are experiencing. Then some tests can be run to get a definitive diagnosis.7Wittram, C., & Weisbrod, G. L. (2002). Mycobacterium avium complex lung disease in immunocompetent patients: radiography–CT correlation. The British Journal of Radiology, 75(892), 340-344. These include:
Chest X-Rays & Especially CT Scans:
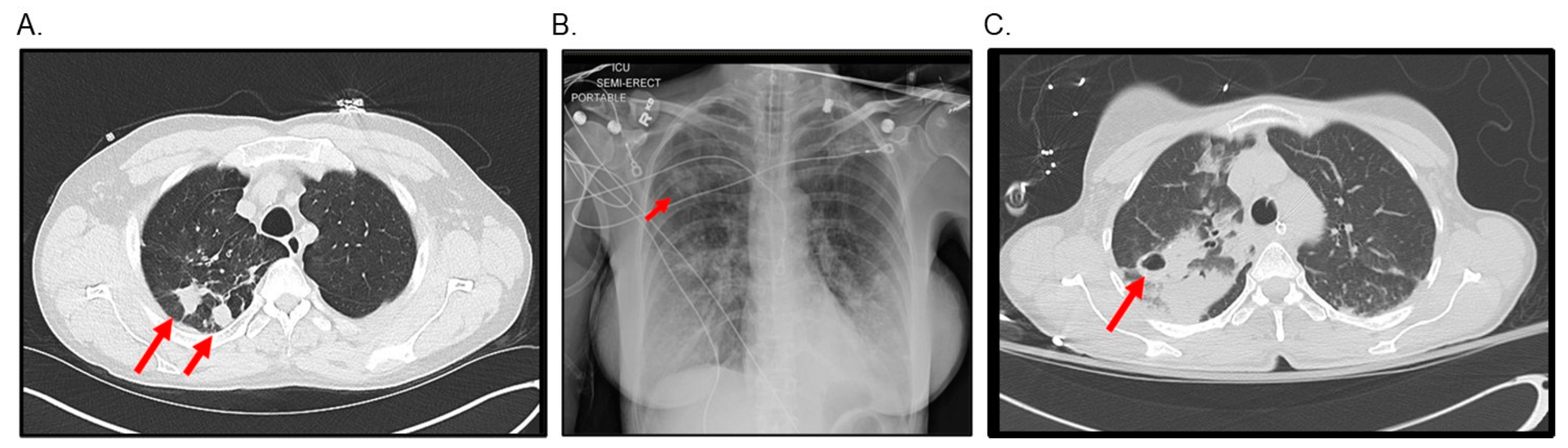
These can detect changes that can occur in the lungs when infection occurs. The amount of changes that occur can tell about how much damage has occurred and treatment plans can be modulated accordingly. Some of the diagnostic characteristics of patients with MAC lung disease are indistinct nodules(swellings), bronchiectasis (abnormal widening of the bronchi or their branches, causing a risk of infection), middle lobe of the lungs being a little more dominant. Overinflation may or may not occur. CT scans provide more detailed information about the extent of the disease and help in assessing the treatment response.8Hendrix, C., McCrary, M., Hou, R., & Abate, G. (2023). Diagnosis and Management of Pulmonary NTM with a Focus on Mycobacterium avium Complex and Mycobacterium abscessus: Challenges and Prospects. Microorganisms, 11(1), 47.
Sputum Cultures (Lung Excretions):
This is done to see if MAC is growing continuously or not. We are all exposed to MAC bacteria daily especially if we are in places where there is soil. Therefore, more than one test is run on different days to boost our confidence that the bacteria is actually coming from your lungs and not from any other external source.
Bronchoscopy:
Bronchoscopy is done when sputum cultures are unable to produce a diagnosis. This procedure involves using a flexible tube to visualize the lungs internally and collect samples directly from the lung tissue.
The diagnostic criteria for nontuberculous mycobacterial (NTM) pulmonary infections include the presence of compatible symptoms, imaging findings consistent with pulmonary disease, and repeated isolation of mycobacteria from sputum (at least two separate specimens) or from one bronchial wash in a patient showing symptoms.9Griffith, D. E. (2024). Overview of nontuberculous mycobacterial infections. UpToDate.
Treatment of MAC Lung Disease
The treatment for MAC lung disease depends on the severity of symptoms.10Pan, S. W., Shu, C. C., Feng, J. Y., & Su, W. J. (2020). Treatment for Mycobacterium avium complex lung disease. Journal of the Formosan Medical Association, 119, S67-S75. Not all individuals diagnosed with MAC pulmonary disease require immediate treatment. Given the prolonged duration of antimycobacterial therapy and its potential side effects, a conservative approach with close observation is often recommended, especially in patients with mild disease. The treatment approach is discussed below:
Watchful Waiting:
Those people who have minimal symptoms and minimal radiographic changes may not need treatment with antibiotics initially. Regular follow-up with breathing tests and sputum cultures is enough. Sputum cultures are typically repeated every two to three months, with imaging performed after approximately six months to monitor disease progression. If bacterial load increases or if radiographic changes such as cavitation or worsening nodularity occur, treatment initiation is recommended.
Airway Clearance:
Airway clearance therapies help remove sputum and bacteria from the lungs, primarily in patients with bronchiectasis (the widening of the airways). These therapies include various breathing treatments, such as those delivered through a nebulizer, and devices designed to help clear sputum from the lower airways.
Medications:
If airway clearance alone is not enough, antibiotics may be prescribed. The decision to treat using antibiotics depends on many variables. a three-drug regimen; macrolide, rifamycin, and ethambutol should be followed. Treatment starts after a shared decision-making discussion with your specialist.
Bacteria can develop antibiotic resistance, which means the drugs can not kill them. So, to help lower the risk of antibiotic resistance while effectively killing the bacteria, you will have to take three different antibiotics for 12 to 18 months. Inhaled antibiotics for people whose infection doesn’t respond to other antibiotics within six months can also be used.
Surgery:
In cases where antibiotics fail, surgery, such as a lobectomy, may be considered. After this procedure, patients may question whether they can continue to live with one lung. The answer is typically yes, but it requires careful monitoring and lifestyle adjustments to maintain health and function. Post-surgery, antibiotics may still be needed to clear lingering bacteria, and the patient must be closely monitored for any complications
Prevention
Though MAC lung disease is not easy to cure and treatment takes a long time, it surely is preventable. Prevention is always better than cure. Here’s what you can do to prevent getting this lethal infection
- Avoid systems that redistribute hot, steamy water, as MAC can thrive in these environments. Ensure that bathroom and kitchen vents are properly used to eliminate steam.
- Make sure you wear masks when you are working in the garden.
- Wear gloves whenever you are gardening and dampen the potting soil before working with it.
Is MAC Lung Disease Contagious?
MAC is not at all contagious. Most people do think it is because it is related to the tuberculosis germ. MAC microbes live in soil and water from which they can be breathed in or ingested. The condition can, however, affect more than one family member at a time, so people tend to assume it is contagious. Some experts are of the view that certain people have a genetic change (mutation) that can make them more prone to MAC infections.
Complications
MAC lung disease can lead to complications like severe wasting, hepatomegaly, splenomegaly, generalized lymphadenitis, and joint inflammation (synovitis or tenosynovitis). In addition to lung involvement, MAC can spread throughout the body, particularly in individuals with advanced AIDS, leading to disseminated MAC disease. Lymphadenitis is common in young children with MAC infections.11Ayoade F, Cotelingam J, Joel Chandranesan AS. Disseminated Mycobacterium avium-Intracellulare Complex Infection Presenting With Disseminated Intravascular Coagulation in an AIDS Patient. J Investig Med High Impact Case Rep. 2017 Nov 14;5(4):2324709617740904. doi: 10.1177/2324709617740904. PMID: 29164156; PMCID: PMC5692144.
Patients with chronic lung conditions, such as bronchiectasis or COPD, are also at increased risk for other respiratory infections, like tuberculosis or pulmonary aspergillosis.
MAC Lung Disease & Covid 19
Mac lung disease puts a person at risk of certain conditions. This includes firstly a decreased protective ability of the respiratory cilia. Cilia is like tiny hair in your bronchi that protects by trapping any dust particles or microorganisms so they do not enter the lungs. Secondly, there is a decreased cytokine response. Cytokines are substances produced by your body during an inflammatory response. They then allow your immune system to set in motion to defend against germs or other substances that can make you sick after entering your body.
Other respiratory infections, such as pulmonary tuberculosis and pulmonary aspergillosis, often occur in patients with Non-Tuberculous Mycobacterium Pulmonary Diseases because of certain chronic structural lung diseases like bronchiectasis, asthma, and chronic obstructive pulmonary disease (COPD). Considering these facts i.e. impaired mucociliary function, weakened immunity, and coexisting structural lung diseases in patients with NTM-PD, the incidence of covid 19 increases. This is the reason why these patients need to be vaccinated earlier because the risk of getting COVID-19 is higher.
MAC Lung Disease & Cancer
There is a strong relationship between MAC lung disease and lung cancer.12Tamura, A., Hebisawa, A., Kusaka, K., Hirose, T., Suzuki, J., Yamane, A., … & Takahashi, F. (2016). Relationship between lung cancer and Mycobacterium avium complex isolated using bronchoscopy. The Open Respiratory Medicine Journal, 10, 20. . Studies show that MAC lung disease can contribute to the development of lung cancer. When MAC infects the bronchial cells, granulomas—clusters of white blood cells and macrophages—form. Over time, this leads to bronchial destruction and the progression of MAC lung disease. The clinical course of MAC is often prolonged, and during this time, chronic inflammation can play a role in cancer development.
Conclusion
Mac lung disease is an infection caused by bacteria found in soil and water. It affects those especially who have compromised immune systems. With strong immunity and good hygiene, we can protect ourselves from this deadly disease. Since the diagnosis is a little difficult, the disease progresses until finally a diagnosis is made. This is why it becomes difficult to treat and even takes a lot of time, resulting in poor lung health. Other diseases like the covid and lung cancer can then affect the person’s health badly.
Refrences
- 1Kumar K, Loebinger MR. Nontuberculous Mycobacterial Pulmonary Disease: Clinical Epidemiologic Features, Risk Factors, and Diagnosis: The Nontuberculous Mycobacterial Series. Chest. 2022 Mar;161(3):637-646. doi: 10.1016/j.chest.2021.10.003. Epub 2021 Oct 8. PMID: 34627854.
- 2American Lung Association. (n.d.). MAC lung disease. https://www.lung.org/lung-health-diseases/lung-disease-lookup/mac-lung-disease#:~:text=MAC%20lung%20disease%20is%20an,be%20referred%20to%20as%20MAI.
- 3Griffith, D. E., Aksamit, T., Brown-Elliott, B. A., Catanzaro, A., Daley, C., Gordin, F., Holland, S. M., Horsburgh, R., Huitt, G., Iademarco, M. F., Iseman, M., Olivier, K., Ruoss, S., von Reyn, C. F., Wallace, R. J., & Winthrop, K. (2007). An official ATS/IDSA statement: Diagnosis, treatment, and prevention of nontuberculous mycobacterial diseases. American Journal of Respiratory and Critical Care Medicine, 175(4), 367–416. https://doi.org/10.1164/rccm.200604-571ST
- 4Lim J, Lyu J, Choi CM, Oh YM, Lee SD, Kim WS, Kim DS, Lee H, Shim TS. Non-tuberculous mycobacterial diseases presenting as solitary pulmonary nodules. Int J Tuberc Lung Dis. 2010 Dec;14(12):1635-40. PMID: 21144251.
- 5Cappelluti E, Fraire AE, Schaefer OP. A case of “hot tub lung” due to Mycobacterium avium complex in an immunocompetent host. Arch Intern Med. 2003 Apr 14;163(7):845-8. doi: 10.1001/archinte.163.7.845. PMID: 12695276.
- 6Lee, S. Y., Kim, J. H., Kim, Y. J., & Kim, S. Y. (2019). Estrogen and Mycobacterium avium complex lung disease: Insights from clinical and animal studies. Journal of Thoracic Disease, 11(1), 1-7. https://doi.org/10.21037/jtd.2019.12.58
- 7Wittram, C., & Weisbrod, G. L. (2002). Mycobacterium avium complex lung disease in immunocompetent patients: radiography–CT correlation. The British Journal of Radiology, 75(892), 340-344.
- 8Hendrix, C., McCrary, M., Hou, R., & Abate, G. (2023). Diagnosis and Management of Pulmonary NTM with a Focus on Mycobacterium avium Complex and Mycobacterium abscessus: Challenges and Prospects. Microorganisms, 11(1), 47.
- 9Griffith, D. E. (2024). Overview of nontuberculous mycobacterial infections. UpToDate.
- 10Pan, S. W., Shu, C. C., Feng, J. Y., & Su, W. J. (2020). Treatment for Mycobacterium avium complex lung disease. Journal of the Formosan Medical Association, 119, S67-S75.
- 11Ayoade F, Cotelingam J, Joel Chandranesan AS. Disseminated Mycobacterium avium-Intracellulare Complex Infection Presenting With Disseminated Intravascular Coagulation in an AIDS Patient. J Investig Med High Impact Case Rep. 2017 Nov 14;5(4):2324709617740904. doi: 10.1177/2324709617740904. PMID: 29164156; PMCID: PMC5692144.
- 12Tamura, A., Hebisawa, A., Kusaka, K., Hirose, T., Suzuki, J., Yamane, A., … & Takahashi, F. (2016). Relationship between lung cancer and Mycobacterium avium complex isolated using bronchoscopy. The Open Respiratory Medicine Journal, 10, 20.





