Tetany is a medical condition caused by an involuntary muscle spasm or contractions, often resulting from electrolyte imbalance and deficient calcium levels in the blood. These spasms can range from mild to severe and can affect various muscles in the body. The causes of tetany can vary from person to person. Tetany, sometimes called smasmophilia, is the hyperexcitability of the nervous system, especially the portion that controls the skeletal muscle movements.1Morris, Noah. “Tetany.” Postgraduate Medical Journal 12.123 (1936): 6.
Symptoms of Tetany
Symptoms of tetany vary in severity and presentation depending on individual factors and underlying conditions. Some common and severe symptoms are listed below.
Common Symptoms
Common mild symptoms of tetany include:
- Muscle spasms, cramps, and twitching
- Numbness around the mouth
- Paraesthesia which is a tingling, numbness, or “pins and needles” around hands and feet
Severe Symptoms
Sometimes, there can be severe symptoms of tetany as well. Understanding these varying degrees of symptomatology is pivotal in effectively addressing the condition’s severity and implementing appropriate interventions. Some pronounced symptoms of tetany are:
- Bronchospasm is when the muscles that line your bronchi (airway in your lungs) tighten, leading to difficulty in breathing.
- Laryngospasm occurs when the vocal cords suddenly spasm or involuntarily contract or seize. As a result, the airway is temporarily blocked, making breathing and speaking difficult, which leads to high-pitched sounds while breathing (i.e., laryngeal stridor)
- Generalized painful muscle cramps
- Carpopedal Spasms are involuntary muscle contractions that primarily affect the muscles of the hands (carpo-) and feet (pedal-), resulting in a claw-like appearance. 2Ito, Nobuaki, and Seiji Fukumoto. “Symptoms and management of tetany.” Clinical calcium 17.8 (2007): 1234-1239.
- Vomiting and nausea can occur because of electrolyte imbalance, which leads to gastrointestinal disturbances. Additionally, muscle spasms associated with tetany can affect the muscles of the abdomen, resulting in vomiting.
- Seizures can cause temporary abnormality in muscle tone, control, and movements.
- Cardiac Arrhythmias occur when the heartbeat becomes irregular, with a problem in the rate or rhythm of the heartbeat.
- Rhabdomyolysis is a severe outcome of tetany, which is rare but can be life-threatening. It involves the breakdown or death of muscle tissue, which releases proteins and electrolytes into the bloodstream. These substances can inflict damage on the heart and kidneys, potentially leading to permanent disability or even death.3Jiwa FH, van den Hoek K, van Zeijl CJJ, Kooter AJ. A Patient with speechlessness and rhabdomyolysis: a rare presentation of severe hypocalcaemia. BMJ Case Rep. 2020 Dec 13;13(12):e238072. doi: 10.1136/bcr-2020-238072. PMID: 33318252; PMCID: PMC7737021.
Symptoms of tetany may be intermittent or persistent, and their severity may fluctuate over time. Factors such as stress, physical activity, and diet may also affect the symptoms, frequency, and severity of tetany.
Causes of Tetany
In general, electrolyte imbalance is the most common cause of tetany. The primary cause is a disruption in the delicate balance of Calcium and other electrolytes in the bloodstream. Understanding these contributing elements is crucial in elucidating the etiology of this condition.
Types of electrolyte imbalance that can cause tetany.
Hypocalcaemia
It is when the levels of calcium are too low in your blood. Calcium plays a crucial part in our body. It helps the nerves work and subsequently contract the muscles. Other uses of calcium are making the heart function and helping in blood clotting.
The causes of hypocalcemia are:
-
Inadequate Dietary Intake
A diet low in calcium intake can lead to hypocalcemia and tetany. It is more common in individuals with limited access to dairy products, green leafy vegetables, and other calcium sources.
-
Malabsorption Disorders
A condition affecting calcium absorption in the bloodstream, especially gastrointestinal diseases like Crohn’s Disease, Celiac disease, and surgical resection of the intestine, can impair the absorption of calcium and other nutrients.
-
Vitamin D Deficiency
Vitamin D is vital for the absorption of calcium in the intestines. Deficiency of Vitamin D, whether due to less exposure to sun, impaired activation in the body, or poor dietary intake, can result in decreased calcium absorption, resulting in hypocalcemia
-
Parathyroid Gland Disorders
The parathyroid glands play a key role in regulating calcium levels in the body by secreting parathyroid hormone (PTH). Dysfunction or removal of these glands due to surgery, autoimmune disorders, or genetic conditions involving the parathyroid gland (e.g., DiGeorge Syndrome) can disrupt calcium homeostasis, leading to hypocalcemia and tetany. 4Fong, Jeremy, and Aliya Khan. “Hypocalcemia: updates in diagnosis and management for primary care.” Canadian Family Physician 58.2 (2012): 158-162.
-
Medication
Some drugs like diuretics and antiepileptics like phenytoin can cause impaired absorption and metabolism of calcium, thus causing hypocalcemia and tetany.
Hypokalemia
Low potassium levels in the body cause hypokalemia. Potassium is vital for muscle functioning, especially heart muscle.
Hypomagnesemia
Hypomagnesemia occurs due to low levels of magnesium in the blood. Magnesium is vital for bodily functions.
Metabolic Alkalosis
Normal physiological pH in humans is 7.35 to 7.45. The human body’s acid-base (pH) balance is critical for well-being. A pH increase of more than 7.45 secondary to any metabolic condition is metabolic alkalosis. It is due to an excess of bicarbonates in our body fluids.
Respiratory Alkalosis
Respiratory alkalosis is a pathology secondary to hyperventilation. It occurs when one breathes too fast or too deeply, causing the lungs to get rid of too much carbon dioxide.
Diagnosis of Tetany
Diagnosing tetany is a comprehensive evaluation of clinical findings, medical history, physical examination, and laboratory tests. Healthcare providers may use the following approach to assess and diagnose a tetany case properly.
Clinical Assessment
The patient will be asked about his medical history and the complaint he presented with. Doctors will then perform a thorough physical examination to assess signs of muscle spasms, hyperexcitability, and other neurological symptoms. Patients may also be asked about their dietary habits, any medical illnesses, and recent surgeries for proper diagnosis.
Laboratory Tests
Laboratory tests are crucial for the correct diagnosis of tetany. Generally, levels of calcium and other electrolytes will be tested and recorded. The normal range of blood calcium levels is from 8.5 to 10.2 mg/dL (2.13 to 2.55 mmol/L). However, normal value ranges may vary slightly among different laboratories. Additional tests, including measurement of parathyroid hormone (PTH), vitamin D levels, and renal function tests, may be performed to identify the underlying cause of hypocalcemia and tetany.
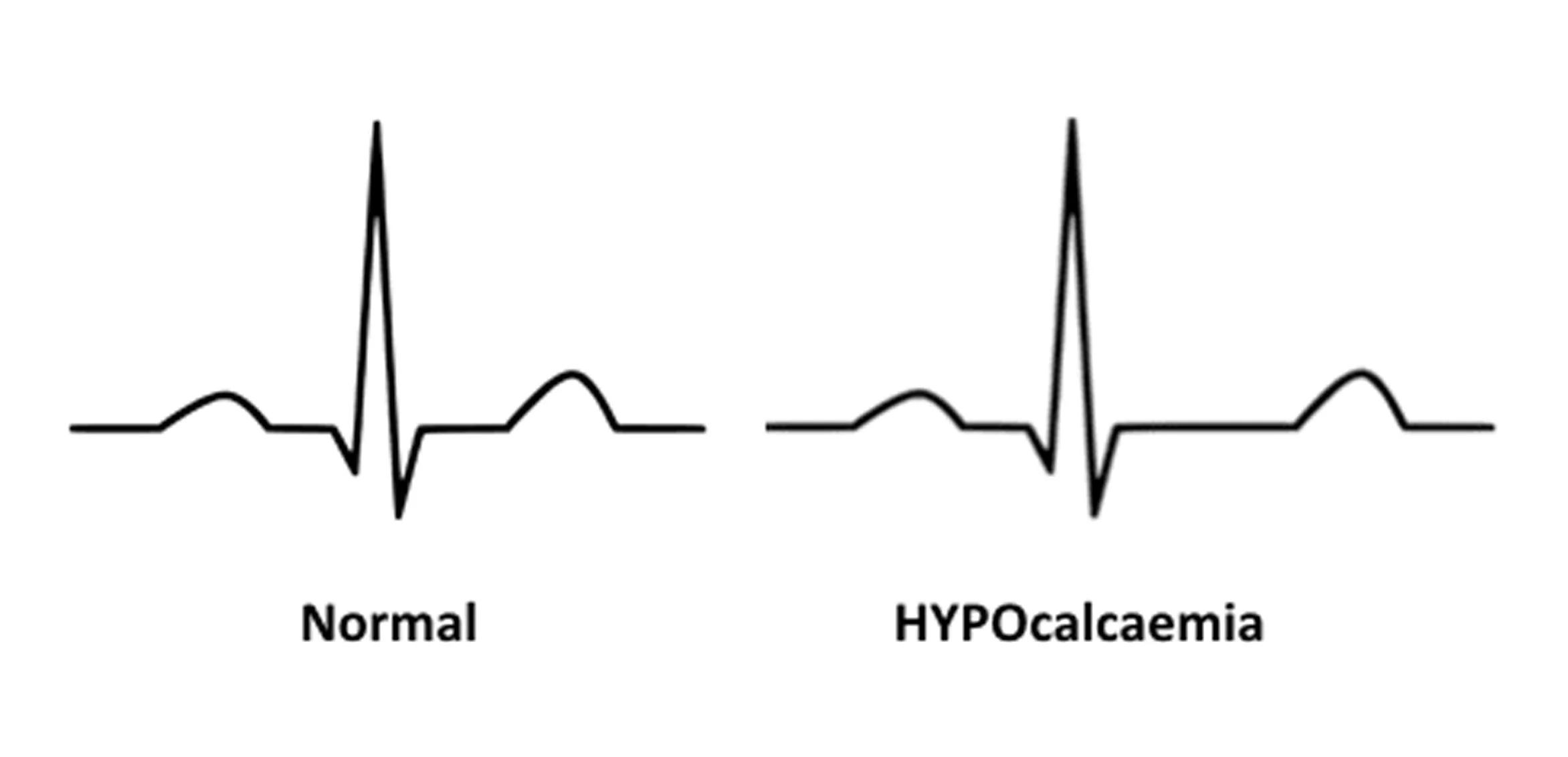
Electrocardiogram (ECG)
The doctor will evaluate the proper heart functioning and detect any abnormalities associated with electrolyte imbalance by performing electrocardiography. It has been speculated that these ECG abnormalities may be attributed to coronary artery spasm. Most commonly, the characteristic ECG manifestation of hypocalcemia is a prolongation of the QT interval because of the lengthening of the ST segment. 5Lehmann, Günter, et al. “ECG changes in a 25-year-old woman with hypocalcemia due to hypoparathyroidism: Hypocalcemia mimicking acute myocardial infarction.” Chest 118.1 (2000): 260-262. 6Slovis, Corey, and Richard Jenkins. “Conditions not primarily affecting the heart.” Bmj 324.7349 (2002): 1320-1323.
Treatment of Tetany
Treatment of tetany aims to correct the underlying medical condition, restore normal electrolyte levels, alleviate symptoms, and prevent complications. The treatment approach may vary from individual to individual depending on the severity and frequency of tetany episodes. Treatment modalities of tetany include:
Oral Calcium Supplements
Administering oral calcium supplementation is usually the first step to treating tetany caused by hypocalcemia. This prevents recurrent tetany episodes. The two main formulations of oral calcium supplements are carbonate and citrate. Other forms of calcium in supplements include gluconate and lactate.
Intravenous Calcium
In acute cases of tetany with severe symptoms or life-threatening complications, intravenous calcium administration may be necessary to rapidly raise blood calcium levels and stabilize the patient. Calcium chloride formulation is preferred for patients in cardiac arrest and other serious cases.
Magnesium Supplements
It is important to check magnesium levels during calcium repletion, as magnesium deficiency is a common cause of treatment-resistant hypocalcemia.
Vitamin D Therapy
Vitamin D is essential for calcium absorption through the intestine, so in case of vitamin D deficiency, Vitamin D2 or D3 should be given according to the patient’s needs.
Dietary Modification
A well-balanced diet is the key to preventing episodes of acute and mild tetany. Thereafter, eating foods rich in electrolytes, such as green leafy vegetables, fortified foods, and fortified beverages, can fulfill the body’s micro mineral requirements and help meet daily nutrient requirements.
Treating Underlying Conditions
To effectively manage tetany, it is necessary to treat the underlying medical conditions such as malabsorption disorders, renal insufficiency, or parathyroid gland problems. Additionally, patients may require hormonal therapy, nutritional support, and even surgery to prevent the recurrence of tetany.
Monitoring & Follow-up
Patients with recurring tetany will need regular monitoring of serum electrolytes. Patients with chronic episodes may require long-term follow-up and periodic laboratory testing.
Latent Tetany
Latent tetany is a subclinical form in which clinical signs are not evident. We can elicit these signs during stimulation. The patient may experience mild symptoms and muscle irritability, but it does not cause significant discomfort. However, it may indicate an underlying electrolyte imbalance that needs warrant and intervention.
Identifying and treating latent tetany is important to prevent the progression of severe tetany and minimize the risks and complications. Therefore, the healthcare provider may suggest lifestyle changes, oral supplementations, and dietary modifications.
What is Trousseau’s Sign?
Trousseau’s sign is observed in patients and unmasks latent tetany in people with no visible symptoms of tetany and hypocalcemia. The blood pressure cuff is inflated, blocking the brachial artery (the main blood vessel of the arm). As a result, the wrist and forearm muscle spasm.7Patel M, Hu EW. Trousseau Sign. [Updated 2023 May 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK557832/
Difference between Tetany and Tetanus
Confusion may occur due to similar-sounding words, such as tetany and tetanus, but they are completely different diseases. They are distinct medical conditions with different causes, symptoms, and treatments.
| Tetany | Tetanus | |
| Definition | Tetany is muscle twitching and spasms. | Tetanus is an infection. |
| Cause | Primarily caused by hypocalcemia. It can also be because of other electrolyte imbalances. | Caused by the bacterium Clostridium tetani, which produces a neurotoxin that affects the nervous system. |
| Symptoms | Muscle twitching, cramps, spasms, numbness or tingling sensations, and muscle stiffness. | Symptoms include muscle stiffness, particularly in the jaw (lockjaw), neck, and abdomen, as well as difficulty swallowing, muscle rigidity, and painful muscle contractions. 8 Cook, T. M., R. T. Protheroe, and J. M. Handel. “Tetanus: a review of the literature.” British journal of anaesthesia 87.3 (2001): 477-487. |
| Treatment | Focuses on correcting hypocalcemia and other electrolyte discrepancies. | Administration of tetanus antitoxin, antibiotics to eradicate the bacterial infection, and supportive care to manage symptoms and complications. |
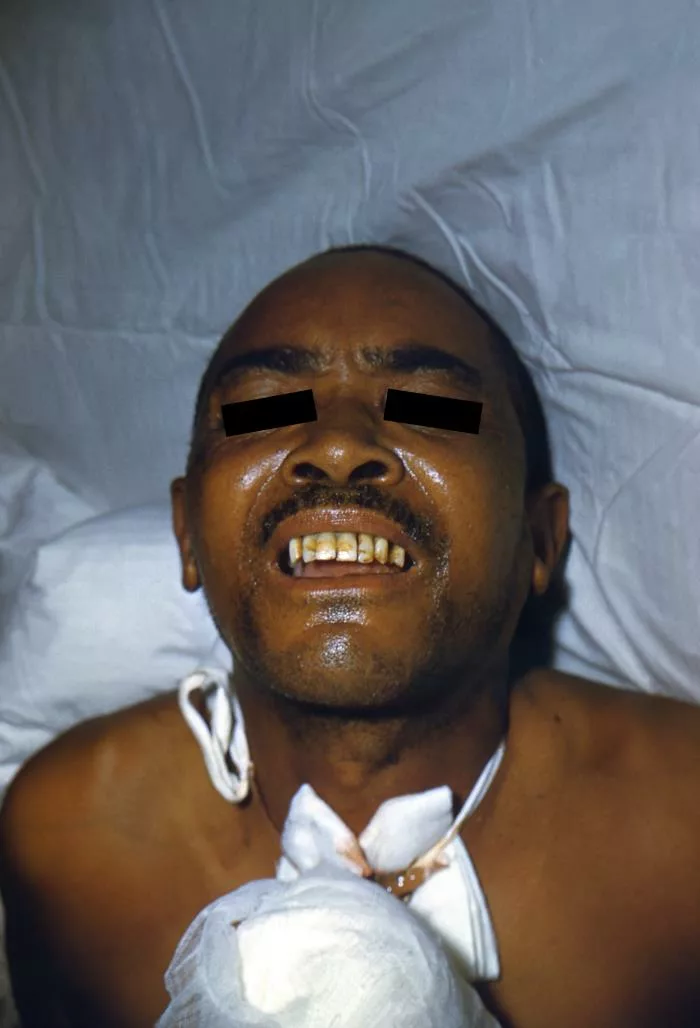
In summary, tetany and tetanus may have some similar symptoms, but they are very different medical conditions with distinct pathophysiology and treatment strategies. Understanding the differences between tetany and tetanus is essential for accurate diagnosis and appropriate management.
Conclusion
Tetany is a medical condition characterized by involuntary muscle spasms and cramps. By understanding, symptoms, diagnosis, and treatment strategies healthcare providers can effectively manage the problem and improve patient outcomes.
Refrences
- 1Morris, Noah. “Tetany.” Postgraduate Medical Journal 12.123 (1936): 6.
- 2Ito, Nobuaki, and Seiji Fukumoto. “Symptoms and management of tetany.” Clinical calcium 17.8 (2007): 1234-1239.
- 3Jiwa FH, van den Hoek K, van Zeijl CJJ, Kooter AJ. A Patient with speechlessness and rhabdomyolysis: a rare presentation of severe hypocalcaemia. BMJ Case Rep. 2020 Dec 13;13(12):e238072. doi: 10.1136/bcr-2020-238072. PMID: 33318252; PMCID: PMC7737021.
- 4Fong, Jeremy, and Aliya Khan. “Hypocalcemia: updates in diagnosis and management for primary care.” Canadian Family Physician 58.2 (2012): 158-162.
- 5Lehmann, Günter, et al. “ECG changes in a 25-year-old woman with hypocalcemia due to hypoparathyroidism: Hypocalcemia mimicking acute myocardial infarction.” Chest 118.1 (2000): 260-262.
- 6Slovis, Corey, and Richard Jenkins. “Conditions not primarily affecting the heart.” Bmj 324.7349 (2002): 1320-1323.
- 7Patel M, Hu EW. Trousseau Sign. [Updated 2023 May 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK557832/
- 8Cook, T. M., R. T. Protheroe, and J. M. Handel. “Tetanus: a review of the literature.” British journal of anaesthesia 87.3 (2001): 477-487.

