Bronchopulmonary dysplasia is a chronic problem that affects the lungs, mostly developed after birth. The term ‘bronchopulmonary’ is related to the lungs, while ‘dysplasia’ means an abnormal change.
Bronchopulmonary dysplasia is not present at birth but is a consequential change due to factors like infections, mechanical ventilation, and even breathing conditions. Preterm infants (especially newborns born before 32 weeks of gestation) are at the highest risk of developing this condition.
While bronchopulmonary dysplasia is lifelong, most newborns often grow up to lead a normal healthy life through proper care and monitoring.
What is Bronchopulmonary Dysplasia?
It is a change rather than a disease. Hence, after stressful conditions, the newborn’s lungs become inflamed and ultimately develop scarring. When looking under the microscope, bronchopulmonary dysplasia presents as damaged lung tissue with enlarged spaces in the alveoli (air sacs of lungs), with a structural change in the small vessels called capillaries, along with increased cellularity.1Coalson, J.J., 2006, August. Pathology of bronchopulmonary dysplasia. In Seminars in perinatology (Vol. 30, No. 4, pp. 179-184). WB Saunders. These changes are irreversible and cause difficulty in breathing.
Bronchopulmonary Dysplasia Signs & Symptoms
All the symptoms are usually termed under the category of respiratory distress. Some common symptoms include:
Rapid Breathing
Since the oxygen supply is limited due to altering breathing, the infants breathe quicker to accommodate this. Rapid breathing itself can lead to various symptoms like:
- Grunting sounds
- Fatigue
- Flaring up of nostrils
Cyanosis
Cyanosis is bluish skin discoloration due to a lack of oxygen in the blood.
Wheeze
Wheeze is a whistling sound produced by the lungs during inhalation and exhalation. Since infants use a lot of force to draw the air into the lungs and even expel it, this creates resistance and difficulty breathing, resulting in wheezing. Neonates (less than four weeks old) born prematurely can wheeze at follow-up, even after two years.
Cough
Coughing is a common symptom and is often accompanied by crackling sounds when using a stethoscope to auscultate the chest, all indicative of fluid build-up and inflammation.
Failure to Thrive
Fragile lungs make breathing an extremely difficult job, and since the energy reserve of infants is greatly affected, this makes the feeding process very difficult. The neonates can’t get appropriate nutrition and ultimately become weak.
Increased Risk of Infections with Bronchopulmonary Dysplasia
Due to difficulty breathing and reduced nutrition, the infant’s immunity often becomes compromised, greatly increasing the risk of certain infections like pneumonia.
Bronchopulmonary Dysplasia in Adults
Most adults are often neonatal survivors of this condition. Since it’s a permanent change, many bronchopulmonary dysplasia adults often present with similar symptoms as neonates. However, the severity varies based on the treatments being received. Like smoking, increased exposure to air pollution, accompanying lung infections, and reduced immunity can aggravate symptoms in adulthood. 2Cassady, S.J., Lasso-Pirot, A. and Deepak, J., 2020. Phenotypes of bronchopulmonary dysplasia in adults. Chest, 158(5), pp.2074-2081.
Apart from this, certain conditions during adulthood, like cystic fibrosis, chronic obstructive pulmonary disease (COPD), idiopathic pulmonary disease, and even cancer, can cause this dysplastic change.
What Causes Bronchopulmonary Dysplasia?
Bronchopulmonary dysplasia is the most common lung problem in childhood. The exact cause is not known. However, certain conditions increase the risk of developing dysplasia. Premature birth (37 weeks or less) and low birth weight (less than 2 pounds) are the two most common causes.
Since the neonates are not fully developed, they are often placed inside the ventilators until gestation, weakening their lungs. Forced ventilation through mechanical ventilation and concentrated oxygen therapy exposes the lungs to great stress, which ultimately destroys the alveoli leading to scarring.
Another commonly associated condition, acute respiratory distress syndrome (ARDS), often leads to bronchopulmonary dysplasia. Although not all neonates with ARDS develop dysplasia, a great risk exists since these neonates have underdeveloped lungs and are premature.3Tao, Y., Han, X. and Guo, W.L., 2022. Predictors of Bronchopulmonary Dysplasia in 625 Neonates with Respiratory Distress Syndrome. Journal of Tropical Pediatrics, 68(3), p.fmac037.
In ARDS, a protein called surfactant is missing, which keeps the lungs moist and the alveoli open. Because of this, neonates often need a mechanical ventilator which helps with breathing.
Diagnosis
If a neonate requires assisted breathing for more than 28 days, we often suspect bronchopulmonary dysplasia. The doctor will usually begin with a clinical assessment looking at the birth weight and prematurity status, followed by a chest examination. Ultimately your doctor will order the following tests for further confirmation:
Blood Tests
A special blood test called pulse oximetry is ordered to calculate the amount of oxygen in the blood. Neonates often have low oxygen saturations.
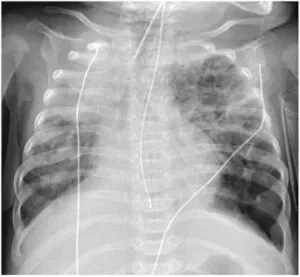
Chest X-Ray
A series of radiations are used to see the neonate’s lung to look for any inflammation, scarring, or changes, all of which are positive for bronchopulmonary dysplasia.4Semple, T., Akhtar, M.R. and Owens, C.M., 2017. Imaging bronchopulmonary dysplasia—a multimodality update. Frontiers in medicine, 4, p.88.
Echocardiography
An ultrasound of the heart is rarely ordered to help look for congenital heart problems that could lead to lung dysplasia.
Pulmonary Function Tests
Bronchopulmonary dysplasia in adults requires monitoring via lung function tests. It usually uses an instrument called a spirometer, which contains balls and a mouth pipe. The patient blows the air through the pipe and tries to lift the colored balls. Hence, this exercise helps assess lung status by allowing the lungs to open up.
Treatment for Bronchopulmonary Dysplasia
Since oxygen worsens this condition, the main aim of the treatment is to get the patient off of supplemental oxygen and promote breathing on their own. The most commonly used treatment options include:
- Provide appropriate nutrition by increasing the calories. Improved nutrition gives the neonate enough energy to grow and breathe independently.5Miller, A.N., Curtiss, J., Taylor, S.N., Backes, C.H. and Kielt, M.J., 2023. A review and guide to the nutritional care of the infant with established bronchopulmonary dysplasia. Journal of Perinatology, 43(3), pp.402-410.
- Reducing fluid overload through medicines like diuretics helps reduce inflammation.
- Maintaining hygiene and following septic measures like using antibiotics to reduce infection risk.
- In case of airway constrictions, bronchodilator drugs can be used. This help opens and relax the breathing muscles and structures, which reduces exertion.
Depending upon the damage, the neonates can take months to even half a year to breathe independently and fully.
What can You Do to Manage it at Home?
Since bronchopulmonary dysplasia has no cure, it often requires lifelong routine changes to help manage it. Some ways to make sure your child stays healthy are:
- Staying up to date with all the vaccinations.
- Making sure everyone in the house gets vaccinated for the flu regularly.
- Avoid exposure to smoke, fumes, and air pollution.
Prevention
The best way to prevent bronchopulmonary dysplasia is to avoid premature birth.
To understand it, we need to understand what causes premature birth exactly.
Some common causes are:
- During pregnancy, avoid smoking and alcohol.
- Maintain a healthy lifestyle.
- Attend all of your antenatal visits regularly.
Another way to prevent the risk of developing dysplasia is to give steroid injections to ARDS patients within seven days. 6Mammen, M.J., Aryal, K., Alhazzani, W. and Alexander, P.E., 2020. Corticosteroids for patients with acute respiratory distress syndrome: a systematic review and meta-analysis of randomized trials. Pol Arch Intern Med, 130(4), pp.276-286.
Conclusion
Bronchopulmonary dysplasia is a permanent condition and can often be quite challenging. Despite having no exact cause, prematurity remains its number one risk factor.
As a parent, your focus should be to ensure your child continues to breathe independently, and with proper care and lifestyle changes, most individuals can lead a normal life.
Refrences
- 1Coalson, J.J., 2006, August. Pathology of bronchopulmonary dysplasia. In Seminars in perinatology (Vol. 30, No. 4, pp. 179-184). WB Saunders.
- 2Cassady, S.J., Lasso-Pirot, A. and Deepak, J., 2020. Phenotypes of bronchopulmonary dysplasia in adults. Chest, 158(5), pp.2074-2081.
- 3Tao, Y., Han, X. and Guo, W.L., 2022. Predictors of Bronchopulmonary Dysplasia in 625 Neonates with Respiratory Distress Syndrome. Journal of Tropical Pediatrics, 68(3), p.fmac037.
- 4Semple, T., Akhtar, M.R. and Owens, C.M., 2017. Imaging bronchopulmonary dysplasia—a multimodality update. Frontiers in medicine, 4, p.88.
- 5Miller, A.N., Curtiss, J., Taylor, S.N., Backes, C.H. and Kielt, M.J., 2023. A review and guide to the nutritional care of the infant with established bronchopulmonary dysplasia. Journal of Perinatology, 43(3), pp.402-410.
- 6Mammen, M.J., Aryal, K., Alhazzani, W. and Alexander, P.E., 2020. Corticosteroids for patients with acute respiratory distress syndrome: a systematic review and meta-analysis of randomized trials. Pol Arch Intern Med, 130(4), pp.276-286.

