Cervical Myofascial Pain Syndrome is considered a public health problem by the National Health Survey 1Capó-Juan, M.A., 2015, January. Cervical myofascial pain syndrome. Narrative review of physiotherapeutic treatment. In Anales del sistema sanitario de Navarra (Vol. 38, No. 1, pp. 105-115). A significant number of medical visits in the orthopaedics clinic which occur as a result of muscle pain are due to myofascial pain (MPS). Cervical MPS affects both men and women; however, it is more prevalent in women than males. This condition may affect 65% of adult women and 37% of adult males with pain 2Borg-Stein, J., 2002. Cervical myofascial pain and headache. Current pain and headache reports, 6(4), pp.324-330
What is Cervical Myofascial Pain Syndrome?
Cervical myofascial pain syndrome 3Touma, J., May, T. and Isaacson, A.C., 2018. Cervical myofascial pain. is a type of musculoskeletal disorder that occurs in the neck and the shoulder region. Myofascial pain means pain that arises from a muscle and its surrounding fascia (connective tissue). Cervical myofascial pain, therefore, implies pain that arises from the muscles and surrounding fascia that support the neck and the shoulder region.
Cervical myofascial pain syndrome most commonly affects the supraspinatus, infraspinatus, trapezius, levator scapulae, and rhomboid muscles. Anyone can occasionally suffer from neck pain after over-exhausting the neck muscles. However, what differentiates cervical myofascial pain from the rest is that it persists and worsens.
Causes & Risk Factors
Pain from Cervical MPS occurs due to a sensory response generated by myofascial trigger points. These focal tender points occur as a result of hypercontracted muscle tissue. The hyper-contracted muscles consist of taut bands within the skeletal muscle that constricts the blood flow leading towards ischemia (restricted blood flow and thus oxygen). Prolonged ischemia eventually causes muscle injury releasing inflammatory products such as cytokines, bradykinins, substance P, potassium, and ATP. As a result, these taut bands form latent and later active myofascial trigger points that produce pain on compression. A doctor can also determine these myofascial trigger points with the help of a myofascial pain syndrome trigger points chart. There are several reasons which can stimulate this mechanism, such as:
Low-Level Muscle Contractions
Low-level muscle contractions are involuntary and weak contractions that can be likened to muscle twitches. These contractions involve the activation of smaller motor units before or after the larger ones. Specifically, the smaller motor units, consisting of type I muscle fibers, are continuously engaged and become overworked due to prolonged activity. This overload on the smaller motor units leads to a metabolic burden. Consequently, an autogenic destructive process called the Cinderella process may be triggered, resulting in the characteristic pain associated with myofascial pain syndrome (MPS). In simpler terms, low-level muscle contractions strain certain muscle fibers, leading to pain commonly experienced in MPS.
Direct Trauma
Active or latent myofascial trigger points may develop from direct trauma. Such trauma can injure the skeletal muscle of the shoulder and neck so that its sarcoplasmic reticulum (cell membrane of skeletal muscle cells) is damaged, releasing calcium and leading to a high calcium concentration within the muscle. This can overstimulate the actin and myosin filaments, eventually leading to a shortage of ATP (adenosine triphosphate). This may damage the calcium pump within the injured muscle, further increasing the calcium concentration and creating a vicious cycle. Eventually, this will form taut bands inside the muscle, which will be the pioneers of myofascial trigger points.
Muscle Contractures
Poor posture of the neck can produce prolonged contractures in the neck muscles. This further develops into taut bands and later trigger points.
Stress & Anxiety
Anxiety and stress are major risk factors for developing cervical MPS 4Ohrbach, R. and Michelotti, A., 2018. The role of stress in the aetiology of oral parafunction and myofascial pain. Oral and Maxillofacial Surgery Clinics, 30(3), pp.369-379. . People who suffer from stress or anxiety might clench their muscles frequently and for longer periods. This can produce a repeated strain on the muscle leading to the development of trigger points.
Signs & Symptoms
Myofascial pain syndrome symptoms vary for each person. Some patients may experience acute pain or a flare-up of symptoms, while others complain of constant dull aching pain. Some typical signs of cervical myofascial pain syndrome include:
- Deep aching and throbbing pain in the neck and shoulders
- Tights or stiffness in the neck and shoulders
- A knot in the neck or shoulder muscles represents a trigger point that is painful to touch
- Tenderness or soreness
- Affected muscles may have weakness and decreased range of motion (e.g., the patient might not be able to rotate his or her shoulder completely).
- Patients may also complain of experiencing other health problems such as headaches, fatigue, poor sleep, anxiety, stress, and depression.
How is Myofascial Pain Syndrome Diagnosed?
Myofascial pain syndrome can be tricky to diagnose. Unlike most diseases, MPS does not come up in lab tests, blood work, biopsy, or imaging tests (although they may be used to rule out a differential diagnosis). Neither does it present with any visible signs such as muscle warmth, redness, or swelling. The actual diagnosis of MPS lies in physical examination. A medical professional will detect MPS by examining the affected muscles and looking for taut bands. The healthcare professional will apply pressure to different trigger points, and the subsequent pain, either at the spot or some distance away (referred pain), will help diagnose Myofascial pain syndrome.
While diagnosing MPS, a healthcare professional aims to examine four different types of trigger points:
- Active trigger point: Lies within the affected muscle, and compression leads to local or regional pain
- Latent trigger point: Represents a dormant trigger point that has the potential to activate
- Secondary trigger point: Present in another muscle that does not contain the active trigger point. But stimulation can elicit the same pain as the functional trigger point.
- Satellite trigger point: A trigger point that is overlapped with a part of another trigger point and, as a result, is inactive
Difference between Myofascial Pain Syndrome and Fibromyalgia
The difference between MPS and fibromyalgia sometimes gets confusing as they both produce a similar type of pain. Moreover, they both consist of trigger points that cause pain. Therefore, a clear difference between the two disorders is very important for an accurate diagnosis.
Fibromyalgia (unlike MPS) is not restricted to one region. Pain from fibromyalgia is migratory and affects both muscles and joints (unlike MPS, which only affects muscles). Pain from fibromyalgia can be felt on both sides of the body as well as above and below the waist. Some researchers believe that fibromyalgia is an aggravated form of MPS, and others believe that it affects how the brain interprets pains by amplifying pain sensory signals.
Treatment
Treatment for myofascial pain syndrome can vary from medications to exercise to different therapies. It is essential to provide symptomatic treatment to a patient with MPS.
VA rating stands for “Veterans Affairs Rating” and determines the percentage of disability an affected individual may have after a medical evaluation. Myofascial pain syndrome VA rating can be assigned with 10%. This means chronic pain resulting from MPS has the potential to severely disable the patients’ life making myofascial pain syndrome treatment a necessity. The two main ways through which treatment is provided are the following. 5Borg-Stein, J. and Iaccarino, M.A., 2014. Myofascial pain syndrome treatments. Physical Medicine and Rehabilitation Clinics, 25(2), pp.357-374. .
1) Myofascial Pain Syndrome Medications
To treat pain caused by MPS, there are oral medications as well as trigger point injections. Some common medications prescribed to patients with MPS are:
- Pain killers
Drugs such as naproxen sodium, and ibuprofen have proven to be effective in treating pain from MPS. They are available OTC (over the counter). Certain painkillers are also available in a skin patch form. - Tranquilizers
Sedatives such as clonazepam have proven to improve symptoms of anxiety and poor sleep that often accompany MPS. Caution should be taken while taking sedatives, as the patient might form a dependency on them. - Antidepressants
Antidepressants such as amitriptyline have been effective in relieving pain and improving sleep in patients with MPS.
2) Myofascial Pain Syndrome Therapies
Apart from medication, the following therapies can be used.
- Physical Therapy
Physiotherapy Physical therapy can be an effective way to treat pain arising from MPS. A physiotherapist can help you learn exercises and techniques to cope with it.

- Needle Procedure
Through a process called dry needling, MPS can be treated by inserting needles around the trigger point and inside it. This works by breaking up the tension inside the muscle. A steroid can also be injected into the trigger point to numb the pain arising from MPS.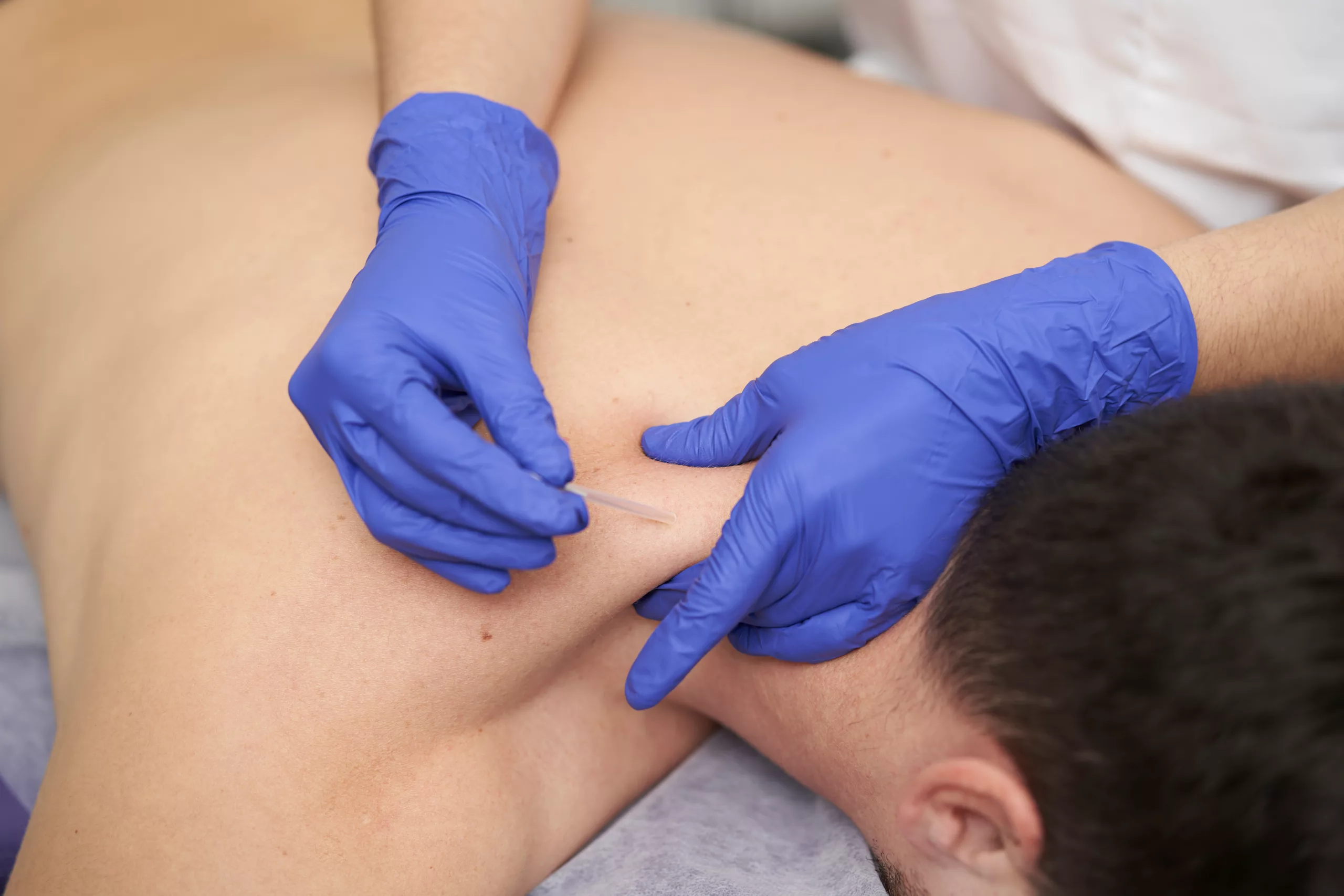
Dry needling in Trapezius Muscle - Ultrasound Therapy
This is a non-invasive yet effective method to relieve pain from MPS. Ultrasound therapy relieves myofascial pain by generating deep heat, increasing circulation, improving tissue flexibility, providing analgesic effects, and enhancing the penetration of topical medications. It promotes healing, reduces inflammation, relaxes muscles, and interrupts pain signals. Proper administration by a healthcare professional is essential.
Prevention
Avoiding triggers and risk factors like stress, anxiety, excessive injury, and poor posture can help reduce the risk of MPS. Always stretching before and after any physical exercise, increasing hydration, and maintaining a good posture are key factors in preventing MPS.
Conclusion
Cervical MPS is a chronic illness that presents with localized pain in the neck and shoulder region of the body. MPS most commonly presents during middle age life and can hamper the affected individual’s quality of life. Treatment for MPS includes medications as well as physical therapies.
Refrences
- 1Capó-Juan, M.A., 2015, January. Cervical myofascial pain syndrome. Narrative review of physiotherapeutic treatment. In Anales del sistema sanitario de Navarra (Vol. 38, No. 1, pp. 105-115)
- 2Borg-Stein, J., 2002. Cervical myofascial pain and headache. Current pain and headache reports, 6(4), pp.324-330
- 3Touma, J., May, T. and Isaacson, A.C., 2018. Cervical myofascial pain.
- 4Ohrbach, R. and Michelotti, A., 2018. The role of stress in the aetiology of oral parafunction and myofascial pain. Oral and Maxillofacial Surgery Clinics, 30(3), pp.369-379.
- 5Borg-Stein, J. and Iaccarino, M.A., 2014. Myofascial pain syndrome treatments. Physical Medicine and Rehabilitation Clinics, 25(2), pp.357-374.

