Acute chest syndrome (ACS) is a potentially life-threatening complication of sickle cell disease (SCD) that affects the lungs. A sudden onset of symptoms such as chest pain, shortness of breath, coughing, and fever characterizes ACS. It occurs when sickle-shaped red blood cells (RBCs) get trapped in the small blood vessels in the lungs, leading to inflammation, decreased oxygen supply, and tissue damage.
Sickle cell acute chest syndrome progresses at a higher rate and is the leading cause of mortality due to sickle cell disease1. Friend, A. and Girzadas, D. (2022) Acute chest syndrome – statpearls – NCBI bookshelf. National Library of Medicine. Retrieved March 4, 2023 from https://www.ncbi.nlm.nih.gov/books/NBK441872/.
This article elaborates on everything you need to know about ACS and its management. Let’s read ahead!
Acute Chest Syndrome Causes
ACS can occur in individuals with sickle cell trait or sickle cell disease, but it is more common and severe in those with sickle cell anemia. The main reason for ACS is a vaso-occlusive crisis in the pulmonary blood vessels. Several factors, such as infection, dehydration, high altitude, or blood transfusions, can trigger it.
Multiple factors that can ultimately lead to acute chest syndrome are the following:
Sickle Cell Disease
Patients who have sickle cell disease (SCD) have sickle cell hemoglobin (HbSS) in their red blood cells, due to which cells attain a crescent shape.
Sickle-shaped cells can clog the pulmonary blood vessels, decreasing the blood flow and amount of oxygen reaching the alveoli.
Bone Marrow Necrosis
Bone marrow is a spongy tissue present centrally in bones. Inadequate blood supply leads to bone marrow necrosis. The dead tissue particles may enter venous circulation and into the lungs, blocking the blood vessels.
Infection
Bacterial or viral infections are the most common stimulants of ACS in children. Lung infections, such as pneumonia, are the leading cause of acute chest syndrome in children.
Embolism
Sometimes, a blood clot formed inside veins detaches and reaches pulmonary vasculature, called thromboembolism. Also, fat globules may cling to the blood vessels and cause obstruction, particularly in the lungs. These globules damage the pulmonary blood vessels and cause acute chest syndrome. Fat and thromboembolism are common causes in adults suffering from ACS.
Covid-19
When studying the relationship between Covid-19 and sickle cell disease patients, multiple factors must be considered. Infection due to SARS-CoV 2 can trigger ACS in some patients with sickle cell disease. However, adequate supportive measures help patients recover completely.
Symptoms
Acute Chest Syndrome manifests as variable symptoms in children and adults. In children, common symptoms resemble those of an infection. These include:
- Cough (sometimes with blood)
- Wheezing
- Fever at 101℉ or greater
- Tachypnea (rapid abnormal breathing)
- Shortness of breath
- Hypoxemia.
Adults suffering from acute chest syndrome may present one or more following symptoms:
- Chest pain
- Difficulty in breathing
- Vaso-occlusive pain (acute pain in both limbs and back due to obstruction in blood supply)
- Pleural effusion (Fluid accumulation in the chest cavity)
Diagnosis and Evaluation
Diagnosis requires both clinical evaluation and radiographic verification. Initially, the doctor takes medical history to identify if the patient has sickle cell disease or is exposed to other risk factors. He then examines the patient for the initial symptoms mentioned above. If a patient shows any of the above symptoms or has a history of any disease that triggers acute chest syndrome, the physician proceeds toward further investigations.
Your physician may recommend the following tests or investigational techniques to confirm the disease.
Chest X-ray
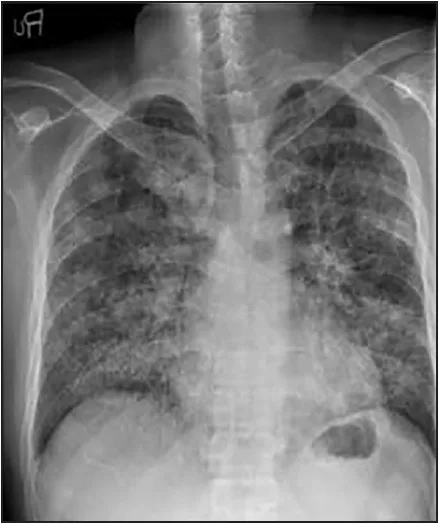
A chest X-ray can help identify lung infiltrates or infections. It shows segmental build-up in the lower parts of the lung and fluid accumulation in the pleura in patients with acute chest syndrome. It also indicates other complications of sickle cell disease, such as rib enlargement or bone infarcts.2Yusuf BJ, Abba AA, Tasiu M. Acute chest syndrome. Sub-Saharan Afr J Med 2014;1:111-8
Computed Tomographic Angiogram (CTA)
Physicians widely recommend using computed tomographic angiograms to analyze pulmonary blood vessels for embolism. CTA makes blood vessels more prominent with contrast3Acute chest syndrome symptoms and diagnosis (2023) American Lung Association. Retrieved March 4, 2023, from https://www.lung.org/lung-health-diseases/lung-disease-lookup/acute-chest-syndrome.
Complete Blood Count
A complete blood count (CBC) test measures the number of red blood cells, white blood cells, and platelets in the blood. When the blood sample is analyzed, a decrease in hemoglobin concentration can suggest the onset of ACS. An increased white blood cell count can indicate a bacterial infection. Platelet count may also be increased as the body tries to repair the damaged blood vessels in the lungs.
Microbial Culture Tests
To look for infection, a microbial culture test may be performed to analyze body fluids, especially blood. Bacteria culture tests can effectively identify the type of bacteria causing an infection. The most common infectious agents causing ACS are respiratory syncytial virus, Chlamydophila pneumoniae, and Mycoplasma pneumoniae.
Pulse Oximetry
The physician recommends Pulse oximetry to assess oxygen saturation in your blood. It involves attaching a device to your index finger to measure the oxygen levels in your blood. It can provide an estimate of the severity of the disease.
What are the Treatment options?
Acute chest syndrome is a rapidly progressing disease and accompanies many complications. Therefore, one should go for aggressive treatment to prevent serious complications, which, otherwise, might be fatal. Physicians may recommend one or more of the following treatment options depending on the cause.
Medications
Various medications, such as Opioid analgesics or Ketorolac, are prescribed to relieve pain. Moreover, Antibiotics are used if a bacterial or viral infection causes ACS. Antiplatelet and Thrombolytic drugs can be prescribed to prevent clot formation. Nitroglycerin is typically used to dilate the blood vessels.
Incentive Spirometer
An incentive spirometer is an accessory device that prevents the lungs from collapsing. It makes your lungs stronger by exercising them. Your physician may recommend an incentive spirometer to free your respiratory tract of secretions. It helps you breathe deeper to get adequate oxygen and avoid respiratory failure.
Blood Transfusion
In some cases, there is a need for blood transfusion also. Patients of sickle cell disease who develop acute chest syndrome may require a blood transfusion in severe conditions.
Supplemental Oxygen Therapy
If a patient has deficient oxygen levels in the blood, additional oxygen therapy is provided. It prevents hypoxia and continuously monitors the blood’s oxygen partial pressure.
Risk Factors
The following conditions are considered to be the risk factors for Acute Chest Syndrome:
- Asthma or other respiratory disorders
- Sickle cell disease
- Severe SCD genotypes, e.g., Hb S-beta⁰-thalassemia
- Genetic predisposition in individuals with HbSS
- Smoking
- Low oxygen levels
- Infection
- Low fetal hemoglobin
- Recent surgery or trauma
Preventive Strategies for Acute Chest Syndrome
Healthcare providers may suggest various preventative measures based on your symptoms and risk factors, such as:
- Taking deep breaths every time you breathe so that air reaches deep down the airway.
- Exercising regularly makes your lungs strong.
- Regular blood transfusion for sickle cell anemia patients.
- Using Incentive Spirometer to help take deep breaths.
Final words
Acute chest syndrome is a life-threatening condition that may lead to respiratory failure. However, you can easily avoid it by taking preventive measures and adopting a healthy lifestyle. Despite all efforts, if you show any of the mentioned symptoms, seek immediate medical help. If diagnosed on time, the disease can be managed effectively. Breathe deeply in the clean air, and stay safe!
Refrences
- 1. Friend, A. and Girzadas, D. (2022) Acute chest syndrome – statpearls – NCBI bookshelf. National Library of Medicine. Retrieved March 4, 2023 from https://www.ncbi.nlm.nih.gov/books/NBK441872/
- 2Yusuf BJ, Abba AA, Tasiu M. Acute chest syndrome. Sub-Saharan Afr J Med 2014;1:111-8
- 3Acute chest syndrome symptoms and diagnosis (2023) American Lung Association. Retrieved March 4, 2023, from https://www.lung.org/lung-health-diseases/lung-disease-lookup/acute-chest-syndrome

