Hyperinsulinemia refers to higher-than-normal (hyper-) insulin levels in the blood (-emia). Produced by the pancreas, insulin is an essential hormone that regulates blood sugar levels by lowering glucose levels. The condition of hormone excess majorly arises due to insulin resistance. Hyperinsulinemia itself is not a disease but rather a sign of an underlying metabolic imbalance. It can be either acute (short-term) or chronic (long-term). Chronic hyperinsulinemia is often associated with serious conditions such as type 2 diabetes, metabolic syndrome, and obesity-related disorders. Generally, it doesn’t cause any noticeable symptoms. However, when arising with metabolic conditions, patients may experience symptoms of prediabetes or diabetes.
Hyperinsulinemia Symptoms
There are no symptoms of excess insulin in the blood. However, the hormone’s excessive availability in the blood removes glucose excessively, leading to hypoglycemia. Thus, patients experience symptoms of hypoglycemia, which include:
- Tremors and body shaking
- Excessive hunger (with cravings for sugar)
- Difficulty concentrating
- Unexplained weight gain (in the long run)
- Anxiety
- Tiredness (and fatigue)
Studies show that patients experience temporary muscle weakness, anxiety, fatigue, thirst, headaches, and shaking due to hyperinsulinemia.1Parker, A. (2020). Hyperinsulinemia. In Encyclopedia of Behavioral Medicine (pp. 1118-1119). Cham: Springer International Publishing.
Hyperinsulinemia Side Effects/Complications
Persistent hyperinsulinemia can both be a trigger and an early indicator of serious conditions like diabetes and metabolic dysfunction.2Thomas, D. D., Corkey, B. E., Istfan, N. W., & Apovian, C. M. (2019). Hyperinsulinemia: an early indicator of metabolic dysfunction. Journal of the Endocrine Society, 3(9), 1727-1747.
Hyperinsulinemia Causes
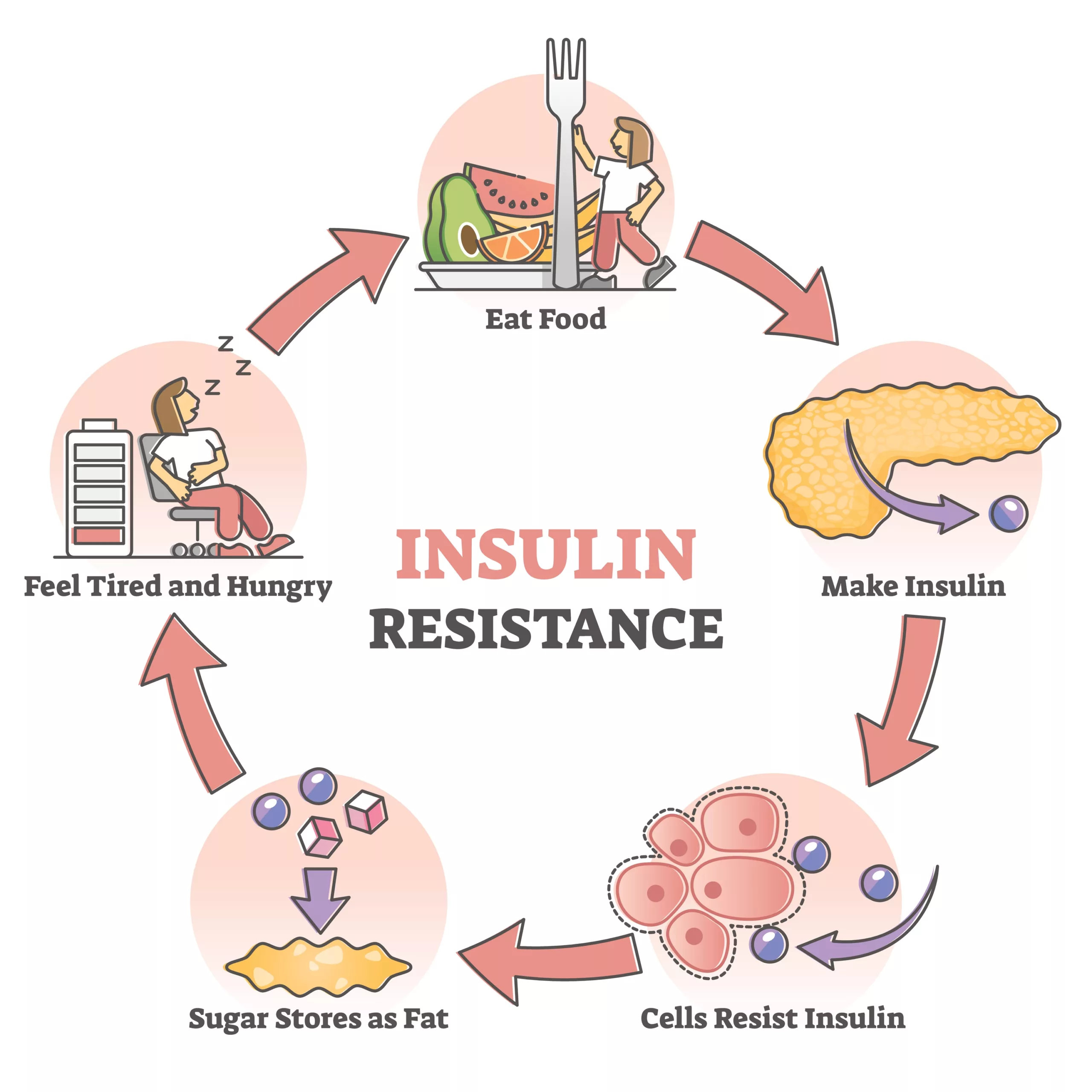
The major underlying cause of hyperinsulinemia is insulin resistance. There are several cases in which the body doesn’t respond normally to the hormone. The incorrect response of the body towards the hormone prompts the pancreas to produce more and more of the protein. Eventually, there is an excess of the hormone in the blood. Clinical studies reveal that insulin resistance can both be a trigger and an effect of hyperinsulinemia.3Shanik, M. H., Xu, Y., Skrha, J., Dankner, R., Zick, Y., & Roth, J. (2008). Insulin resistance and hyperinsulinemia: is hyperinsulinemia the cart or the horse?. Diabetes care, 31(Supplement_2), S262-S268.
Individuals may also develop hyperinsulinemia following gastric bypass surgery. Research suggests that surgeons should be aware of hyperinsulinemic hypoglycemia (with neuroglycopenia) as a complication of Roux-en-Y gastric bypass (RYGB). The procedure leads to negative consequences by bringing changes in the gut hormonal milieu.4Malik, S., Mitchell, J. E., Steffen, K., Engel, S., Wiisanen, R., Garcia, L., & Malik, S. A. (2016). Recognition and management of hyperinsulinemic hypoglycemia after bariatric surgery. Obesity research & clinical practice, 10(1), 1-14.
Sometimes, cancer can also lead to hyperinsulinemia. Insulinoma is a rare pancreatic tumor that may cause recurrent hyperinsulinemic hypoglycemia in patients.5Anlauf, M., Bauersfeld, J., Raffel, A., Koch, C. A., Henopp, T., Alkatout, I., … & Klöppel, G. (2009). Insulinomatosis: a multicentric insulinoma disease that frequently causes early recurrent hyperinsulinemic hypoglycemia. The American journal of surgical pathology, 33(3), 339-346. Another uncommon cancerous condition that may cause surplus hormones in the blood is nesidioblastosis (especially in infants).6Jabri, A. L., & Bayard, C. (2004). Nesidioblastosis associated with hyperinsulinemic hypoglycemia in adults: review of the literature. European journal of internal medicine, 15(7), 407-410.
Risk Groups:
Experts have identified certain groups that have a higher propensity to develop the condition. There are greater chances of developing hyperinsulinemia if you have the following conditions:
- Obesity: A higher-than-normal weight is considered a direct contributor to insulin resistance and consequently to insulin excess. Recent studies have highlighted a two-way relationship between obesity and hyperinsulinemia.7Zhang, A. M., Wellberg, E. A., Kopp, J. L., & Johnson, J. D. (2021). Hyperinsulinemia in obesity, inflammation, and cancer. Diabetes & Metabolism Journal, 45(3), 285-311.
- Visceral fat (fat within your abdominal cavity) is a major contributor to insulin resistance. So, if you have a fatty belly, there is a higher chance of you getting the disorder.
- Black: People (especially children) with black or Hispanic ethnicity have a higher likelihood of developing hyperinsulinemia than individuals of other origins.
Hyperinsulinemia Diagnosis
Hyperinsulinemia is typically diagnosed through a fasting blood test, which measures insulin and glucose levels. Since no standard reference range exists for fasting insulin, doctors assess the results in the context of glucose metabolism and insulin resistance markers.
Differential Diagnosis:
Hyperinsulinemia Vs Hyperinsulinism
While both conditions sound very similar, they are not the same. Hyperinsulinemia only indicates raised insulin levels in the blood, while hyperinsulinism is a manifestation of pancreatic disturbance that leads to too much hormone production. The former arises primarily due to insulin resistance, while the latter is mostly the result of a genetic disorder that impacts the insulin secretion regulatory cells of the pancreas. In most cases, hyperinsulinism is present at birth, i.e., congenital hyperinsulinism, and is frequently associated with serious hypoglycemia.
Hyperinsulinemia Treatment
As hyperinsulinemia is more of a manifestation than a condition, the main aim of the treatment is to manage the underlying issues (insulin resistance or insulinoma, etc.). Doctors adopt measures to clear insulin from circulation while improving overall insulin sensitivity. In most cases, clinicians do not prescribe medications and recommend that patients adopt lifestyle/dietary changes only. Steps that can help clear the excess hormone include:
- Eating a balanced diet
- Performing exercise daily
- Losing weight and reducing belly (visceral) fat
You can try aerobics (cardio) and resistance exercises like walking, jogging, etc., to strengthen your muscles and reduce body fat. These exercises have a cumulative effect on the insulin sensitivity of the muscles and the rest of the body.
Medical Treatment for Severe Cases
In cases where hyperinsulinemia results from insulinoma (a pancreatic tumor) or genetic disorders like congenital hyperinsulinism, medical intervention is required:
- Medications such as diazoxide (to reduce insulin secretion) or octreotide (a somatostatin analog that suppresses insulin release) may be prescribed.
- Surgical removal of insulinomas is necessary if a tumor is the underlying cause.8Zhuo F, Menon G, Anastasopoulou C. Insulinoma. [Updated 2025 Jan 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK544299/
- Pancreatectomy (partial removal of the pancreas) may be considered in severe congenital hyperinsulinism cases that do not respond to medication.
Final Word
Hyperinsulinemia is a state of excess insulin in the blood. It is different from insulinism as it mainly develops due to insulin resistance (and not because of pancreatic anomalies). The condition can be acute or chronic. It is mostly asymptomatic. However, the excess circulation of the glucose-maintaining hormone can lead to hypoglycemia and associated symptoms (tremors, confusion, sugar cravings, etc.). Increased insulin resistance (due to obesity and visceral fat), cancer of the pancreas (insulinoma), and gastric bypass surgery can cause surges of the hormone in the blood. Doctors do not prescribe medication for the condition and instead advise patients to reduce weight and body fat by adopting exercise and healthy eating habits. These steps reduce insulin resistance and correct hormone levels.
Refrences
- 1Parker, A. (2020). Hyperinsulinemia. In Encyclopedia of Behavioral Medicine (pp. 1118-1119). Cham: Springer International Publishing.
- 2Thomas, D. D., Corkey, B. E., Istfan, N. W., & Apovian, C. M. (2019). Hyperinsulinemia: an early indicator of metabolic dysfunction. Journal of the Endocrine Society, 3(9), 1727-1747.
- 3Shanik, M. H., Xu, Y., Skrha, J., Dankner, R., Zick, Y., & Roth, J. (2008). Insulin resistance and hyperinsulinemia: is hyperinsulinemia the cart or the horse?. Diabetes care, 31(Supplement_2), S262-S268.
- 4Malik, S., Mitchell, J. E., Steffen, K., Engel, S., Wiisanen, R., Garcia, L., & Malik, S. A. (2016). Recognition and management of hyperinsulinemic hypoglycemia after bariatric surgery. Obesity research & clinical practice, 10(1), 1-14.
- 5Anlauf, M., Bauersfeld, J., Raffel, A., Koch, C. A., Henopp, T., Alkatout, I., … & Klöppel, G. (2009). Insulinomatosis: a multicentric insulinoma disease that frequently causes early recurrent hyperinsulinemic hypoglycemia. The American journal of surgical pathology, 33(3), 339-346.
- 6Jabri, A. L., & Bayard, C. (2004). Nesidioblastosis associated with hyperinsulinemic hypoglycemia in adults: review of the literature. European journal of internal medicine, 15(7), 407-410.
- 7Zhang, A. M., Wellberg, E. A., Kopp, J. L., & Johnson, J. D. (2021). Hyperinsulinemia in obesity, inflammation, and cancer. Diabetes & Metabolism Journal, 45(3), 285-311.
- 8Zhuo F, Menon G, Anastasopoulou C. Insulinoma. [Updated 2025 Jan 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK544299/

