Esthesioneuroblastoma (ENB), also called olfactory neuroblastoma, is a rare malignant nasal cavity tumor originating from the olfactory neuroepithelium. It is an undifferentiated tumor of the olfactory neuroepithelium with neuroectodermal origin. Esthesioneuroblastoma (ENB) is most commonly situated in the upper part of the nasal cavity and is locally aggressive. It can spread via blood and lymph nodes (hematogenous and lymphatic routes, respectively).
Olfactory neuroblastoma is not a gender-specific tumor. It affects both men and women equally. It may occur at any age but most commonly affects young adults. The mean age of presentation of ENB is 40-70 years.
 Since its initial demonstration by Berger and Luc in 1924, thousands of cases have been reported worldwide. Esthesioneuroblastoma accounts for 5% of nasal cavity tumors and 0.3 % of other aerodigestive systems.1Limaiem, F. (2023, January 1). Esthesioneuroblastoma. StatPearls – NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK539694/
Since its initial demonstration by Berger and Luc in 1924, thousands of cases have been reported worldwide. Esthesioneuroblastoma accounts for 5% of nasal cavity tumors and 0.3 % of other aerodigestive systems.1Limaiem, F. (2023, January 1). Esthesioneuroblastoma. StatPearls – NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK539694/
What are the Causes of Esthesioneuroblastoma?
There is no exact known cause of Esthesioneuroblastoma. It occurs due to genetic mutation in normal cells that multiply independently without limitation. Mutation in MYC and KDR genes is also noted in Esthesioneuroblastoma.
What are the Symptoms of Esthesioneuroblastoma?
Symptoms of Esthesioneuroblastoma vary depending on the severity of the disease. The following are a few symptoms of Esthesioneuroblastoma:
- Anosmia ( loss of sensation of smell)
- Epistaxis (Frequent nosebleeds)
- Difficulty breathing because it obstructs the airway
- Headaches
- Visual abnormality
- Orbital pain/pain in the eyes
- Proptosis (Bulging of the eyeball)
- Epiphora (watery eyes)
- Symptoms of Syndrome of inappropriate antidiuretic hormone secretion
Its growth begins in the nasal cavity and extends into the eyes, sinuses, and brain. It can spread into parotid glands and other neck areas via lymph nodes. At advanced stages, it can metastasize into the liver, lungs, brain, and other body parts.
How to Diagnose Esthesioneuroblastoma?
The diagnostic workup of Esthesioneuroblastoma starts with clinical history and general physical examination. Further, radiological investigations help diagnose this malignant tumor. A biopsy is also necessary to determine the histological features of the tumor.
History & Physical Examination
A detailed history of the patient with suspected Esthesioneuroblastoma is critical to make a diagnosis. After taking a thorough history, doctors do a thorough general physical examination to support the diagnosis. The physiological examination includes the following steps:
- Neurological examination (examination of all relevant cranial nerves)
- Ophthalmic examination
- Examination of head and neck
Flexible Endoscopy
A camera-guided flexible endoscopic tube is inserted inside the nose to visualize the interior of the nose. Your doctor can see the extent of the tumor with this technique.
Laboratory Investigation
There are no specific laboratory studies to confirm Esthesioneuroblastoma. Getting the following baseline investigations before surgery is necessary to avoid complications. These are complete blood count (CBC), clotting profile, and serum electrolyte levels.
Radiological Examination
Radiological examination of Esthesioneuroblastoma includes CT scan, MRI, nuclear imaging, and staging. 2Zinaye, A. (2022). Olfactory neuroblastoma. Radiology Reference Article | Radiopaedia.org. https://doi.org/10.53347/rID-9341
- Computed Tomography Scan (CT scan):
X-ray has no role in the diagnosis of Esthesioneuroblastoma. A 3 mm coronal fine-cut CT scan is the radiological investigation of choice. Sinuses and bony erosion on CT scan indicate Esthesioneuroblastoma. - Magnetic Resonance Imaging (MRI):
MRI is preferred when a detailed view is required. It usually shows a hypointense area compared to the surrounding area on a T-1 weighted image, enhanced by gadolinium. It is isointense or hyperintense on T-2 weighted images. MRI provides a better evaluation than a CT scan. - Nuclear Medicine Scan:
These tumors are MIBG-avid, which may be used to differentiate them through meningiomas of the anterior cranial fossa.
Histological Findings
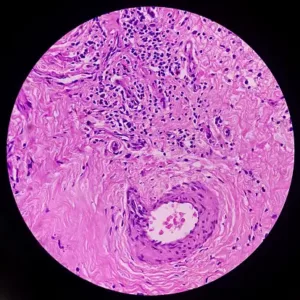
Various histological presentations characterize Esthesioneuroblastoma. The hallmark of these presentations is Rosset or pseudorosette appearance.
TNM-Staging of Esthesioneuroblastoma
Staging of the tumor is an important guide for the treatment therapy and prognosis of the disease. According to the Kadish staging system, Esthesioneuroblastoma is divided into three categories:
1. Group A tumors: Tumor that is limited to the nasal fossa
1. Group B tumors: Tumor that extends into the paranasal sinuses
1. Group C tumors: Tumors that extend beyond paranasal sinuses and nasal cavity
Dulguerov and Calceterra demonstrated the TNM staging system of Esthesioneuroblastoma based on CT scans and MRI findings. The TNM staging system is as follows:
- T1-Tumor involves the nasal cavity and paranasal sinuses, excluding upper ethmoidal cells.
- T2-Tumor that involves the nasal cavity, paranasal sinuses, and erosion of cribriform plate.
- T3-Tumor that extends into orbit, sparing rural invasion
- T4-Tumor involving the brain and its structures
- N0-No nodal involvement
- N1-Cervical lymph nodes involvement
- M0- No distant metastasis
- M1-Distant metastasis is present
Staging:
The following is the staging of Olfactory neuroblastoma, considering its extent, invasion of lymph nodes, and metastasis. Treatment and prognosis of this malignant tumor depend on the staging.3Somenek, M., MD. (n.d.). Esthesioneuroblastoma Workup: Laboratory Studies, Imaging Studies, Histologic Findings. https://emedicine.medscape.com/article/278047-workup#c7
| staging | T | N | M |
| 1 | T1 | N0 | M0 |
| 2 | T2 | N0 | M0 |
| 3A | T3
T1-T3 |
N0 N1 |
M0
M0 |
| 3b | T4 | N0 or N1 | M0 |
| 4A | T1-T4 | N2 | M0 |
| 4B | T1-T4 | N2 | M1 |
Biopsy
Esthesioneuroblastoma appears as a gray-red mass inside the nasal cavity. An intraoperative biopsy is taken under general anesthesia and sent to the lab for further investigations. It is usually performed after the radiological intervention to determine the vascularity of an esthesioneuroblastoma tumor.
How to Treat Esthesioneuroblastoma?
Treatment of the tumor depends upon the severity according to the staging. There are three treatment modalities for Esthesioneuroblastoma.
- Complete surgical removal of the tumor
- Radiation therapy
- Chemotherapy
Sometimes a combination of these treatment modalities is required because treatment with a combined modality has a lower recurrence rate than a single modality.
Surgical Resection
Surgery remains the treatment of choice for Esthesioneuroblastoma, offering the best control of the tumor and a favorable survival rate. When the tumor is small and there is no lymphatic spread or regional metastasis, complete surgical removal is necessary. Transitioning to more advanced cases, when the tumor displays local aggression, endoscopic craniofacial resection becomes imperative. In such instances, the use of endoscopic-assisted surgery is required to effectively remove the tumor, followed by radiotherapy.
It is important to note that surgical resection, while effective, is not without its potential complications. These include cerebrospinal fluid leakage, vision loss, infections leading to abscess formation, and loss of smell. Despite these potential risks, surgery remains a vital approach in managing Esthesioneuroblastoma due to its ability to achieve tumor control and favorable survival outcomes.
Radiation Therapy
Radiation therapy is a technique in which an external beam of <6000 cGy is required to control the tumor with low rates of radiation-induced side effects. The need for radiation therapy depends on the staging and grading of the tumor.
Chemotherapy
Chemotherapy is not required in routine treatment. It is necessary for palliative care or multi-modality care when the disease is more advanced and aggressive. Chemotherapeutic agents that are used in this therapy are:
- Cyclophosphamide
- Vincristine
- Doxorubicin
- Cisplatine
Esthesioneuroblastoma Life Expectancy
The life expectancy of this tumor depends upon the staging of the tumor. The overall 5-year survival rate is:
- Stage 1 -5 years survival rate is 100%
- Stage 2- 5 year survival rate is 89 %
- Stage 3A- 5 years survival rate is 78%
- stage 3B- 5 years survival rate is 60%
- stage 4A- 5 years survival rate is 0%
- stage 4B- 5 years survival rate is 0 %
What is the Prognosis of Esthesioneuroblastoma?
The prognosis of this tumor depends upon its staging and grading. Poor prognostic factors of Esthesioneuroblastoma are :
- High staging
- Distant metastasis
- Age above 50 years and below 20 years
- spread inside the cranium
- highly proliferative
- females
- polyploidy/aneuploidy
Highly proliferative and metastatic tumors at advanced stages in the elderly have a poor prognosis and lower survival rates.
What is the Differential Diagnosis of Esthesioneuroblastoma?
Many other diseases may mimic Esthesioneuroblastoma. Your doctor will suggest different investigations to make a diagnosis. The differentials of this malignant tumor are:
- Rhabdomyosarcoma (is a malignant tumor that forms in soft tissues like muscles, connective tissues, and hollow organs.
- Extramedullary Plasmacytoma (tumor of plasma cells that forms inside soft tissues and outside the bone marrow)
- Mesenchymal Chondrosarcoma (It is a rare and aggressive tumor that is a variant of chondrosarcoma)
- Olfactory Neuroepithelioma (a malignant tumor of the sinonasal tract that originates from olfactory neuroepithelium)
- Meningioma (the most type of brain tumor that arises from the meninges)
- Pituitary Adenoma (benign or non-cancerous growth in the anterior pituitary)
- Juvenile Nasopharyngeal Angiofibroma (A benign or non-cancerous tumor that arises in the nasopharynx and grows behind the nose)
- Small Cell Osteosarcoma (A variant of osteosarcoma characterized by small round cells)
- Lymphoma (Cancer that begins in the lymphatic system of the body)
Clinical signs and symptoms, radiological and histological features differentiate between these tumors and Esthesioneuroblastoma.
Conclusion
To conclude, Esthesioneuroblastoma, also called olfactory neuroblastoma, is an uncommon malignant neoplasm that originates from the olfactory nerve ending. Its treatment and prognosis depend on the staging and grading of the tumor. Surgical resection is the treatment of choice, followed by radiotherapy. Chemotherapy can help at advanced stages. Additionally, the overall survival rate of Esthesioneuroblastoma is five years.
Refrences
- 1Limaiem, F. (2023, January 1). Esthesioneuroblastoma. StatPearls – NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK539694/
- 2Zinaye, A. (2022). Olfactory neuroblastoma. Radiology Reference Article | Radiopaedia.org. https://doi.org/10.53347/rID-9341
- 3Somenek, M., MD. (n.d.). Esthesioneuroblastoma Workup: Laboratory Studies, Imaging Studies, Histologic Findings. https://emedicine.medscape.com/article/278047-workup#c7

